May 28, 2021
TRUENEWSREPORT
BY: STAFF
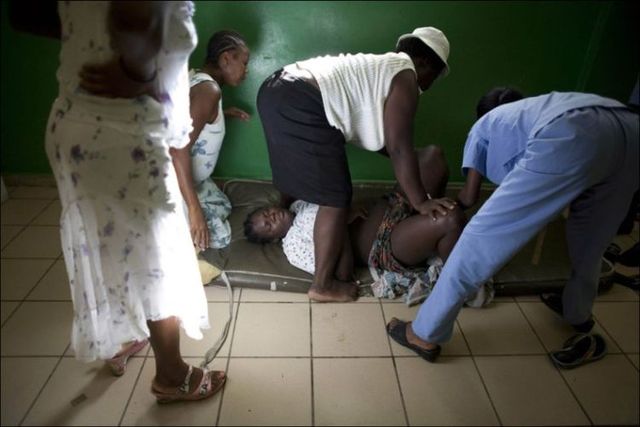
TRUENEWSBLOG – High in the mountains of southeastern Haiti, a woman lay down on the concrete floor at a local non-profit, bleeding profusely as she labored to give birth. The placenta had pulled away from the wall of the uterus and, as she hemorrhaged, the only thing left to do was to get her to the hospital.
The road to the nearest hospital was marked with potholes so large, they could engulf a small car. Nonetheless, the villagers loaded the woman and her husband into the back of a truck, and they took off. Ten minutes later, they returned. Their driver held in his hands a small package — the couple’s stillborn child.
“That story [moved] me to tears and it was really my decision point,” said Valerie Mossman-Celestin, executive director of Haitian Assets for Peace International, or HAPI, a witness. “Something breaks our hearts and it’s a call to action.”
Haitian mothers and their infants die in childbirth at an alarming rate. Five mothers and 47 children will die out of every 1,000, according to the World Factbook and World Population Review respectively. By comparison, the mortality rate in the neighboring Dominican Republic is .95 out of every 1,000 mothers and 17.5 out of every 1,000 children.
In response to the acute need, both Haitian and American-based organizations have been working, in rural pockets and with little fanfare, to help as many mothers and babies as they can reach. One of the larger groups is Midwives for Haiti (MfH), an organization founded by Nadene Brunk Eads in 2006.
Eads, a certified nurse-midwife based in the U.S., saw firsthand the difficulties many Haitian women faced as a medical team volunteer. In 2003, she and a team of midwives and obstetricians began a culturally-appropriate training for skilled birth attendants (SBA), health professionals who provide care during childbirth. Three years later, Eads founded MfH when community leaders in Hinche, a town of 50,000 in the Central Plateau, sought her help.
When it became clear the skilled attendants needed a place to practice, the organization chose nearby St. Therese Hospital, then with its anemic staff of two.
“Today, the organization pays the salaries of 18 skilled birth attendants and operates 24/7,” said Jane Drichta, executive director of MfH.
In 2020, more than 3,100 births took place at St. Therese as attendants worked with the hospital.
Makensia Fontaine, head of the hospital’s maternity ward and staff, defines a good day as when she’s able to do everything in her power for her patients. A bad day is, “when a patient who you should be able to help comes in,” said Fontaine, “but there’s no blood available for a transfusion — and she dies.”
That scenario points to an ongoing need for skilled support throughout the months prior to birth as well. Mothers come to the hospital, but often, like that woman in labor who delivered the stillborn while en route, they wait too long. Many expectant mothers may also be malnourished or have medical conditions like high blood pressure or diabetes. MfH recognized the hospital’s impact on successful deliveries. Nine years later, it established the Carrie Wortham Birth Center in Cabestor, a remote region three hours from Hinche where the maternal mortality ratio was roughly three times the country’s average.
Not long after the Cabestor center opened, a group of 19 people brought in a mother and her newborn, after a five-hour trek over a mountain ridge. Skilled birth attendants removed the mother’s still-attached placenta and saved her life.
Taking medical care to the community
Numerous studies have found that contact with prenatal care professionals reduces mother and infant deaths. For one, prenatal care influences the mother’s choice of where to deliver. Women who receive care early on, especially if they developed a complication, were more likely to deliver at a hospital. Seeing the unmet need, MfH began a mobile clinic program, including a custom-built Jeep driven to various communities to deliver care to expectant mothers, in 2010.
The skilled attendants assessed pregnant and postpartum women. Through simple questions — “How are you feeling?” “Do you have headaches?” “Is your baby moving?” — they come across more complicated issues, such as twins or a low red-blood cell count. “Those everyday conversations … that we have with mothers are the hallmark of midwifery care,” blogged Amy Ginn, a volunteer with MfH.
Attending to a patient and returning a month later was less than ideal. Haiti’s Ministry of Public Health and Population partnered with MfH to create in-place community clinics to improve service and build local trust. By 2019, MfH transitioned its mobile program to reach patients in the permanent settings. Altogether, the organization supports more than 6,000 patients annually through its 22 prenatal and postnatal clinics.
Connecting to the matwòns
While many Haitian women recognize that it’s safer to give birth in a facility, an overarching perception of patient neglect and isolation persists. As a result, many choose to deliver at home.
Expectant mothers turn to matwòns, Haiti’s traditional midwives who attend 60 percent of all Haitian births. Different types of community members — family, neighbors, Vodou priests — fill this niche role.
While most are capable, many matwòns lack some basic knowledge or the safe tools to handle complications, observers say. However, because so many mothers rely on the matwòns, MfH began offering a five-month formal training program to teach them the danger signs and when to recommend that mothers seek additional help, Drichta said.
Graduates of the program receive a certificate of completion and monthly delivery kits that include a sterile blade for cutting the umbilical cord and a device to clamp it. A matwòn demonstrating delivery techniques during MfH training workshop. Photo credit: Cheryl Hanna-Truscott “The training helped me a lot,” said Bernard Forteus, a matwòn.
One mother whose child was delivered at home suffered from severe vaginal tearing. Forteus encouraged the woman to go to the hospital and accompanied her, helping to calm the scared mother as doctors anesthetized her and stitched the tear.
Skilled birthing graduates in demand
MfH now employs 68 Haitians and three international staff. It is on track to graduate 204 attendants total, by the end of this year. Both its classes and practical work have continued through the pandemic, according to Drichta.
Many health clinics seek to hire its graduates, as a result. Mossman-Celestin, of HAPI, said her organization initially did not have a birthing assistance program, but after what they witnessed, they had to help. Recently, HAPI hired two graduates trained in life-saving techniques for mothers and infants. “In the U.S., we have I.V. machines to provide a drip of magnesium sulfate, which must be carefully and precisely administered or it can cause death,” said Mossman-Celestin. “MfH grads learn how to do this manually, counting the drips.” HAPI also employs three nursing assistants, who the Mizak-based nonprofit sent to the MfH course for neonatal resuscitation.
“We have saved many infants thanks to this training and equipment,” said Mossman-Celestin. “That alone helped spread our reputation.” In 2015, HAPI skilled birth attendants delivered eight babies. Last year, they delivered 85. Perrine Stock, clinical director at MfH, has blogged about the impact her organization is having on the ground.
One day, a pickup truck pulled up outside the maternity ward carrying an unconscious woman. The medical team on hand took the steps necessary to stabilize the mother. “All this was achieved in minutes,“ Stock wrote, “and with an efficiency and confidence that made me stop and take stock.”
No emergency buzzer was pressed — they didn’t have one. No multidisciplinary team of experienced professionals rushed in — it didn’t exist. “It was just our [teachers], graduates and students, working to save the life of a woman in grave danger,” said Stock. “And they did – and they do – every single day.”